
Spondylolisthesis - slippage of vertebra
Spondylolisthesis - slippage of vertebra


Condition
Spondylolisthesis means slippage of the spine. Normally, the vertebral bodies in the spine are all well aligned. In some cases one can slip (usually forwards) in relation to the one below it. Depending on the degree of slippage, spondylolisthesis is classified in five slip grades:
Grade 1: <25% Grade 2: 25-50% Grade 3: 50-75% Grade 4: 75-100% Grade 5: complete dislocation (spondyloptosis)
There are a number of possible causes:
- Dysplastic or congenital spondylolisthesis occurs early in life and is related to an abnormal development of the last lumbar vertebra (L5) and / or sacrum during pregnancy. This causes a marked slip in most cases (grade 4 or 5)
- Isthmic spondylolistesis refers to an abnormality of the so-called pars interarticularis. The term spondylolysis is used describe the presence of the defect without slippage. This part of the vertebra connects the upper and lower facet joints. In the majority of cases, this is caused by a fracture of this structure allowing the vertebral body to slip forward. The fracture occurs over a period of time (so-called fatigue fracture) because of repetitive injuries or abnormal forces on the spine. The fracture appears at some point in childhood with subsequent slippage in adolescence. It is uncommon but possible hat the slippage worsens after the age of 20. The most common level (90%) is L5/S1.
- Degenerative spondylolisthesis means slippage due to wear and tear in the spine. It is usually a combination of wear and tear of the intervertebral disc and facet joints which hold the vertebral body in position in relation to the one above and below. This is the most common type of spondylolisthesis and is almost never greater than a grade 1 or 2 slip.
- Traumatic spondylolisthesis can occur after major accidents involving the spine. It can also be a complication after spinal surgery, in particular decompression of the spine (laminectomy) although this is very rare.
- Pathologic spondylolithesis is a rare complication of a variety of diseases involving the vertebra (osteogenisis imperfecta, achondroplasia, Paget disease, metastase and others.
Symptoms
Many patients with spondylolisthesis have no or mild symptoms. However, some experience low back pain, sciatica or symptoms of spinal claudication. In rare cases it can lead to incontinence due to pressure on the bowel and bladder nerves (cauda equina syndrome).
Complications
In some cases the slippage gradually progresses although apart from a very few exceptions (traumatic spondylolisthesis) the spine is not unstable. Prolonged pressure on nerves can damage these and lead to neuropathic pain. The patient experiences a burning sensation in the leg or foot. Once this has occurred it is often difficult to treat. A significant neurological deficit like weakness is uncommon.
Investigations
A thorough history of the symptoms is important to obtain information about the development of the problem. Clinical examination will assess possible sources of the pain and any neurological deficit. Plain x-rays and flexion / extension views will show the degree of slippage and determine whether the slip is stable or not. Special x-rays (oblique views) can show the pars defect. In patients who have symptoms of spinal claudication or sciatica, MRI should be done to see if there is pressure on any nerve. In some cases a CT scan is necessary to look at the bony anatomy in more detail.
Treatment and Outlook
Treatment and outlook depends on many factors like degree of slippage and progression, underlying type and how much problems it is causing for the patient. All patients should be referred for physiotherapy focusing on cores stability exercise. However, physiotherapy will not reverse or even prevent progression of any slippage but can lead to significant improvement of back and leg pain. Spinal manipulation cannot reduce the slippage. Spinal injections (facet or epidural injections might temporarily improve back or leg pain but should not form part of a long term management plan except in a few exceptional cases.
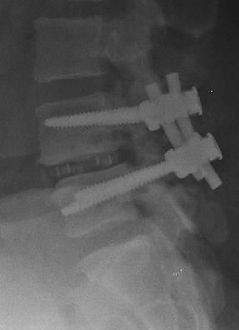
Surgical options include decompression and fusion of the spine (spinal fusion). Which surgical procedure is chosen depends on a number of factors. Most spine surgeons will probably advocate a pedicle screw fixation and (if possible) interbody cage (PLIF,TLIF, XLIF).